Well – it happened again. For the third time in my adult life I found myself recovering from a concussion. It happened in late June, with a less than exciting story of a head impact while loading luggage into a cab. While less aggressive than my previous two from wakeboarding and longboarding, this one was different. It was different not only because the challenges seemed to linger for a longer period of time (thanks, aging!), but also because we as the collective rehabilitation community have learned so much more about what to do for concussion recovery.
Instead of spending a great deal of time being frustrated about the injury (although this certainly did occur), I decided to focus most of my intention and effort on working with the many professionals in our area who I have collaborated with many times in the past. I have always enjoyed trying to learn from the expertise of others, but experiencing their approaches firsthand is an entirely different experience. With the demands of day-to-day life, it is tempting to try to push through recovery and put rehabilitation on the back burner. Between work, family, and life demands, finding the time and motivation to do what is needed to get better is something that can be very challenging to commit to. While concussions certainly do improve with time, when left alone they often heal in much the same way that many other injuries to the body heal – inefficiently and without return to full and complete function. Think about breaking an ankle – if you leave it alone for several months, it will certainly “heal,” yet will likely continue to flare up with exertion and cause issues well into the future if not guided and properly rehabilitated. The brain is no different.
It is important to acknowledge that my experience will not be identical to the experience of others. It is critical to seek the guidance of a rehabilitative specialist to assess where you are in the process and what needs to be done. Below is my journey, and my journey alone – but I hope that it might help others to find their way through what can be a truly unsettling time.
Day 1 – The Injury
Following the impact of my forehead into the taillight of the SUV, an immediate “buzzing” moved from the sight of injury, travelling immediately towards the back of the head. After the initial daze, I collected myself and clumsily guided my body into the back of the vehicle, instinctively and foolishly exclaiming that I was fine. For the remainder of the drive I remember feeling as though there was a wave of light vibrations emanating from my skull and a light magnetic-like outward pull on my brain. I had an immediate instinct that I was concussed, but tried to shrug it off.
Knowing the importance of initiating light motion and movement early on, I fought the urge to sleep and went for a 3 hour walk around the streets of Kelowna. Throughout the walk, I had a very disconcerting sensation that my mind was separate from my body – different from lightheadedness, more as though the wiring that drives movement and thought were completely distinct. As the evening approached, this disconnection between my mind and body seemed to widen. When I finally went to sleep that night, it felt as if my head and body were existing in entirely different parts of the room (I know this sounds strange, but stick with me!).
Day 2: Brain Breaks
Awakening to a feeling that my head was floating about a foot above by neck, I tried to encourage myself to shake it off and face the day. As I prepared to head into the office, I knew I probably shouldn’t go in. But, like many before me, I felt guilt surrounding my many commitments to the day and decided to soldier on. While I took several quiet “brain breaks” in my office with the lights off, going to work was probably the equivalent of trying to run on a recently broken leg – foolish, and very likely to prolong recovery. My words of advice to those struggling with recent head injury is to do all that you can to take 2-3 days of general rest, incorporating walks and light movement into the day, regardless of the perceived cost.
Day 3-4: Glasses, Computer Recommendations, Meditation and Vision Therapy

General recommendations that helped me to manage and avoid headaches during the initial recovery phase were incorporation of blue-light reducing computer software (https://justgetflux.com/), and use of low powered therapeutic glasses on the computer (incorporating prism). It’s important for me to underscore this point – I do not have a traditional glasses prescription, having had perfect “fighter pilot” vision for my entire life. That being said, without the use of therapeutic glasses, I was unable to tolerate reading or computer work for more than 3 minutes without symptom provocation. The tension that they relieved was incredibly marked and profound – so much so that I am still using them to write this very blog.
In addition to the use of therapeutic glasses, I began early on with syntonic phototherapy. This form of vision therapy involves the use of a variety of different wavelengths of light to preferentially stimulate, in my case, the parasympathetic nervous system. If you think it sounds a little odd, all I can say is that throughout my recovery, syntonic phototherapy has subjectively had the most direct and immediate impact on my symptoms of headache and disorientation. We have been using this form of treatment at our office for several years – but to experience the benefit firsthand was incredibly impactful, only deepening my resolve that offering this is in the best interest of our clients.
Along with syntonic phototherapy, a daily practice of meditation helped guide me through the many lows I experienced early on. The app Insight Timer, and the guided meditation “Deep Healing” by David Ji proved to be particularly powerful for me (https://insighttimer.com/davidji/guided-meditations/deep-healing)
Day 5-6: Dietary modifications: drhailey.ca
On the advice of my naturopathic physician, who treats a great deal of concussions herself, I made the transition to the ketogenic diet at around Day 5. While I certainly found a very clear reduction in the sensation of general brain fog, I would be remiss if I didn’t comment on the fact that this is not an overly easy diet to transition towards or adhere to. Preliminary evidence however is demonstrating that ketones may be a more suitable fuel for neural recovery than glucose – so, on the diet I went. My experience while on this diet was on the whole quite positive, aside from the initial 24 hours of light dizziness and fatigue. Be sure to consult your medical professional before leaping into ketosis with both feet.
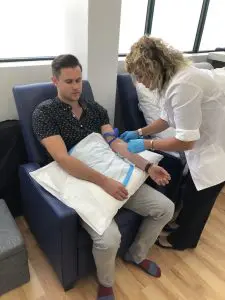
In addition to a ketogenic transition, I was also grateful to receive several glutathione injections, and also incorporated Omega-3, Mito-Matrix and adrenal supplementation into my daily regimen. Glutathione is an extremely powerful antioxidant, and has been used by many to reduce recovery time from concussion and decrease general sensations of brain-fog. I happened to be teaching a weekend course at the time of my injections, and the lunch-time “pick me up” certainly helped me to get through the long and grueling day.
Other important dietary considerations were cutting out alcohol entirely and reducing caffeine intake to one cup per day. I have to be honest about this one though – I did try to have a glass of wine during week one, and it might have been one of the most bizarre experiences of my life. Following injury, the blood-brain barrier tends to be quite permeable and extremely sensitive to the effects of stimulants or depressants. My experience certainly confirmed what I had read on the topic, with one glass feeling much the same an entire bottle. Definitely try to learn from my mistake – cut out the booze entirely, the risk of re-injury is just too high.
Day 7-10: Acupuncture and Fitness: https://momentumkelowna.com/
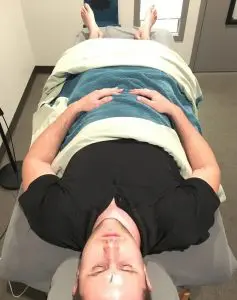
Continuing along the trend of encouraging parasympathetic support to promote healing, I began acupuncture during my second week of recovery. This proved to be hugely beneficial for me – with each treatment leaving me with a minimum of 72 hours of clarity, reduced dizziness and lightheadedness.
In addition to acupuncture, I also began to increase my cardiovascular training. Large scale studies have demonstrated the importance of attempting to return to sub-symptom cardiovascular activity following concussion. Those that do are significantly less likely to find themselves with a chronic diagnosis of post-concussion syndrome. Beyond the initial 72 hours, rest is certainly not best.
Week 2-4: Vestibular Evaluation & Training: https://www.lifemark.ca/Harvey-Avenue

After several weeks of promoting parasympathetically driven healing, along with building cardiovascular tolerance, I was able to get in for a proper vestibular evaluation. It was here that I discovered that I had in fact developed a right unilateral hypofunction (reduction in function of my right vestibular apparatus) – likely an aggravation of a previous deficit from my more aggressive concussion 13 years prior.
Vestibular rehabilitation at its core is about recalibrating the balance system driven by your inner ear. An outline of 5 activities was given to me to perform at home, and although challenging, I noticed a very clear dissipation of lightheadedness throughout my faithful routine of performing them. To be honest, having a diagnosis which justified my symptoms, along with a direction for how to improve, was extremely mentally satisfying for me at this stage of recovery. The frustration of not knowing what’s wrong and being unsure about how to fix it might be one of the most challenging mental hurdles anyone with a concussion must face.
Week 5-7: Getting a little ahead of myself
It’s certainly not uncommon for many people to start feeling like they are coming out of the injury at this point. Generally feeling as though the worst is behind you, it is very common to start pushing yourself more than you probably should. This was very much the case for me. Weeks 5-7 were characterized by a busy work schedule, travel and generally neglecting the rest that my brain still craved. As such, I found myself dip into a period of rather consistent headache – in my case, emanating from the back of my skull.
Week 8: Cervical Evaluation & Treatment: https://www.nuccakelowna.com/
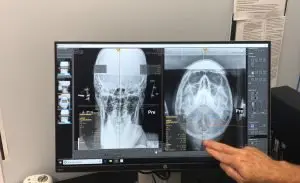
This was a big week for me, as I was finally able to align schedules with a colleague of mine who exclusively practices NUCCA chiropractic. It’s amazing to think back on, but it quite literally took one treatment for me to experience complete dissipation of the headache I had felt for weeks prior. 3 follow-ups were all that was needed to align the slight cervical deviation uncovered at my initial evaluation, and thus a near complete resolution of my lingering concussion symptoms. Magic!
Week 9: Craniosacral: http://physioactivebc.ca/
In order to super-charge the positive impact I experienced with NUCCA chiropractic, it was advised that I attend a few sessions of craniosacral therapy. I don’t pretend to be an expert in this area of rehabilitation, but subjectively I can tell you that it worked wonders for relieving the light vibrational sensations emanating from the top of my skull. It was a very calming experience during the treatment, with positive effects that lingered for weeks after treatment.
Week 10-12: Recovery, Finally.
As I write this, around 3.5 months out from my concussion, it feels rather surreal to reflect on all that I have experienced. I’m ever grateful to the wonderful network of health care providers who have guided me back to fighting form and, in hindsight, feel rather blessed for the experience. Seeing firsthand the impact of many of the treatments outlined above will make me a better practitioner and hopefully allow me to guide people who are struggling in the direction that may benefit them most. Concussions are incredibly scary, and there will undoubtedly be many moments where you feel terrified that you’ll never feel or think like yourself again.
While I am the first to acknowledge that every concussion is extremely unique, I hope my journey helps someone who is reading to chart a path and move in the direction of healing. As stated earlier in the blog, rest is definitely not best – and fortunately, we are spoiled in the Okanagan with providers of specialty services who can stack the odds of complete recovery well in your favour.
Until next month,
Dr. Paul Rollett, OD, FCOVD




